Cancer Screening at NYC, Queens, and Long Island
What does Garden OB/GYN in NYC, Queens, and Long Island do to prevent gynecological cancer?
Cancer screening detects signs of cancer before you have symptoms and while the cancer is still in an early stage. The team at Garden OB/GYN NYC, Queens, and Long Island believes in taking a proactive approach to screening for all types of gynecologic cancers, including ovarian and endometrial cancer.
Why is Cancer Screening Important for My Health?
Cancer screening detects the presence of precancerous and cancerous changes before you develop symptoms. When you get routine cancer screening, your doctor can identify these changes at the earliest possible stage. Early detection makes it possible to provide life-saving treatment. The doctors at Garden OB/GYN NYC, Queens, and Long Island specialize in knowing when to screen for all types of gynecologic cancers. They also have the expertise to detect cancers at an early stage even when standard screening recommendations don’t exist.
How Often Should I Get Screened for Cancer?
Standard screening recommendations state the age at which you should get your first screening and how often you should get tested. However, it’s more important to get a personal screening recommendation. Your doctor at Garden OB/GYN in NYC, Queens, and Long Island determines when you need screening after assessing your overall health and evaluating risk factors such as your family history. You may need earlier and more frequent cancer screenings than the standard recommendations if you have a high risk for a specific type of cancer.
What are the Types of Gynecologic Cancer and How are They Screened?
Gynecologic cancers can develop in your cervix, ovaries, uterus, vagina, vulva, and breasts.
Here’s how these cancers are detected at an early stage:
- Cervical Cancer: Pap smears should be completed each year during a woman's annual examination. A pap smear screens for precancerous or cancerous changes in your cervix. You can also get an HPV test, which reveals whether you have active human papillomavirus (HPV). While HPV causes cervical cancer, an HPV test is primarily a red flag rather than a screening tool. You could have an active virus at the time of your test, then your body could safely clear it out before it causes problems.
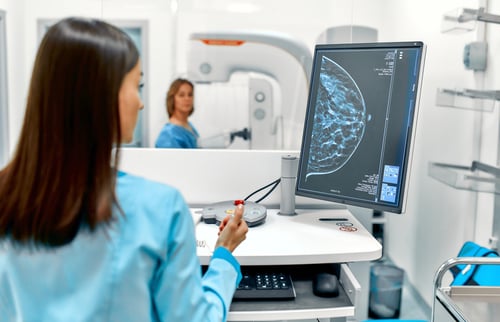
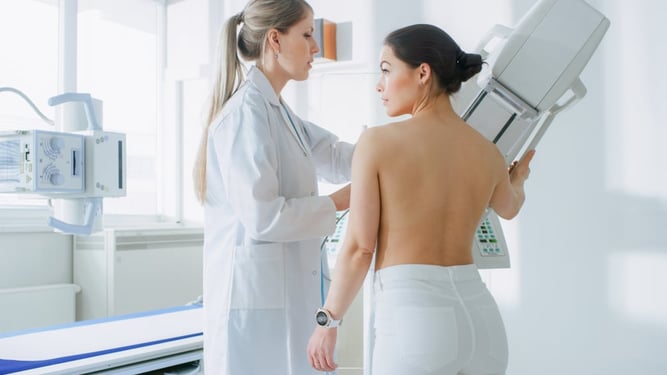
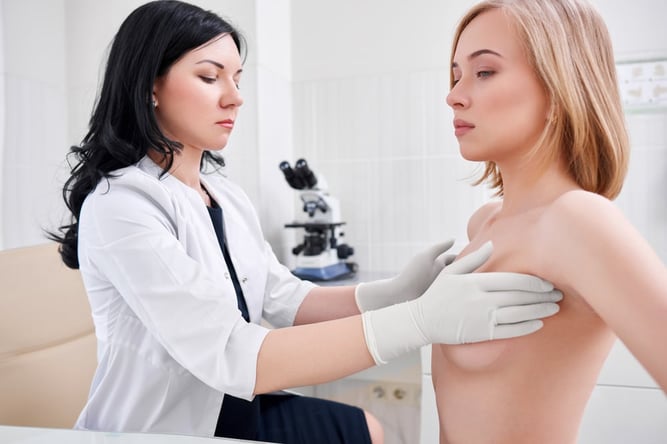
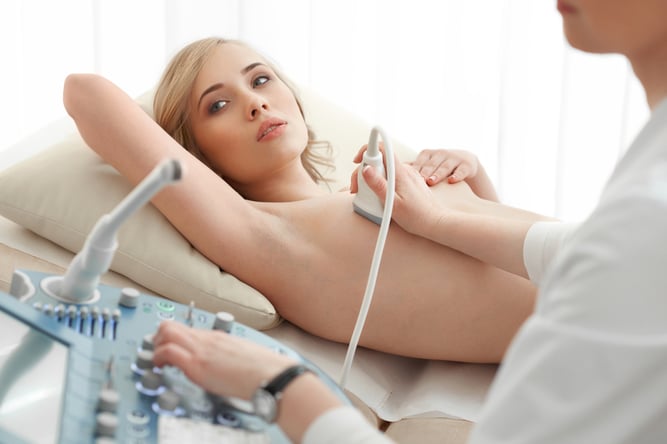
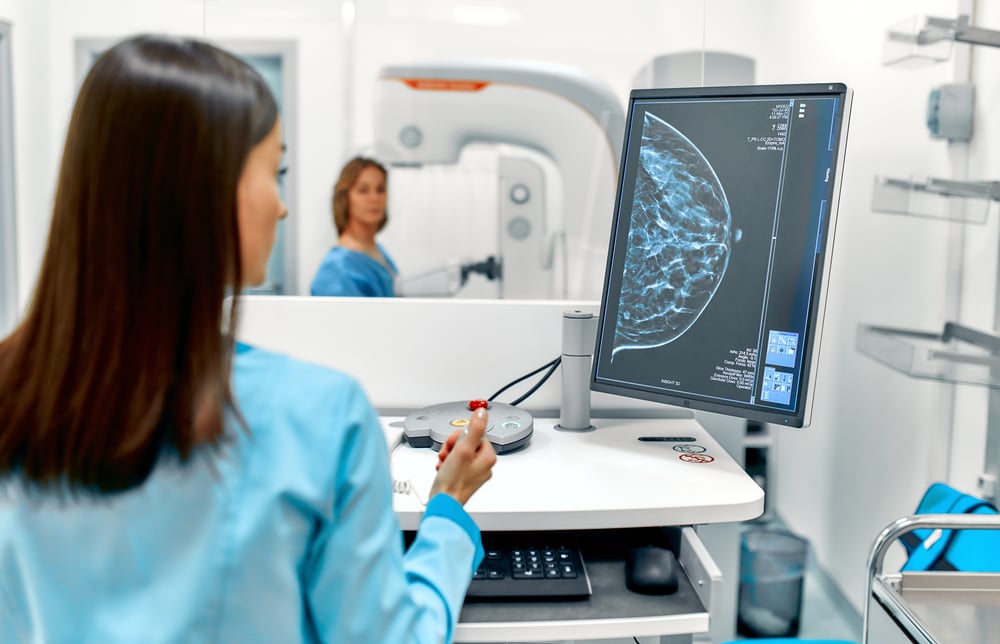
- Breast Cancer: Mammogram, breast ultrasound, MRI, a clinical breast exam, and breast self-exams are all used to screen for breast cancer.
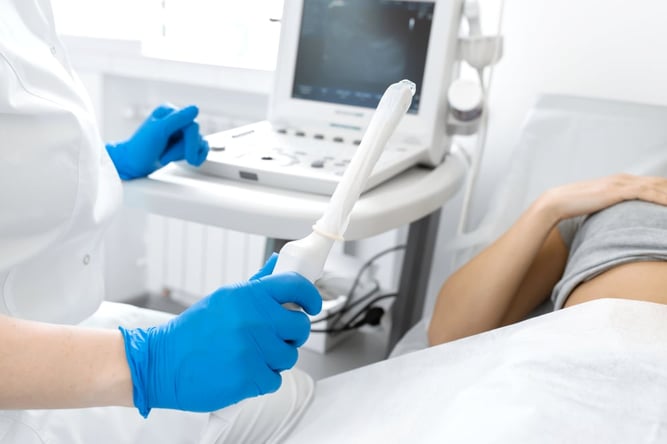
- Ovarian and Endometrial Cancers: There aren’t any standard screening tests for ovarian and endometrial cancers, but the team at Garden OB/GYN at NYC, Queens, and Long Island uses expertise in transvaginal, 3D, and Doppler ultrasound to detect both types of cancer at an early stage. The doctors at Garden OB/GYN believe that transvaginal ultrasound is such an important screening tool that they offer it to all women at their annual well-woman exam. Their proactive approach allows them to detect both cancers at an early stage.
- Vagina and Vulva Cancer: Early signs of vaginal and vulvar cancer are often detected during your routine pelvic exam. When your doctor sees signs of inflammation or cellular changes, they perform a colposcopy. A colposcopy provides a magnified view of your vulva and vagina so abnormal tissues are visible and a biopsy can be performed.
In addition to gynecologic cancers, we also realize the importance of complete cancer screening at any of our office locations, including NYC, Queens, and Long Island.