Cervical Cancer Screening: What You Need To Know.
Cervical cancer is the 4th most common cancer worldwide among women. In the United States, pap smear tests allow us us to decrease the incidence of cervical cancer, and reduce mortality rates associated with cervical cancer.
Cervical cancer is the fourth most common cancer worldwide among women, with approximately 530,000 cases of invasive cervical carcinoma diagnosed annually. In the United States, we have advanced resources available to us to decrease the incidence of cervical cancer, and thus, reduce mortality rates associated with cervical cancer. How do we do this? The Papanicolaou test, a.k.a. the pap smear.
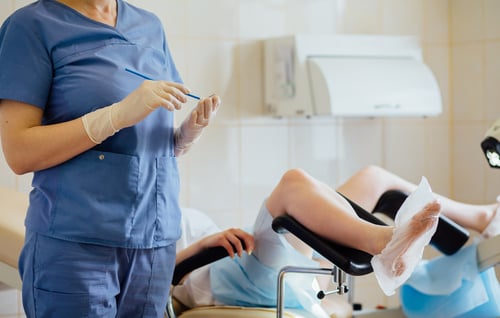
What is a Pap Smear?
Pap smear is the most widely used screening tool to detect abnormal cervical changes and human papillomavirus. Pap smears can identify precancerous and early-stage disease. This is why a routine gynecological exam is so important to maintain and improve your overall health. Pap smears along with HPV vaccination programs are our primary defense against cervical cancer. Being proactive about prevention and screening strategies can help us defeat cervical cancer before it even develops.
What is HPV?
So here is a quick wrap-up of HPV: there are more than 200 types of human papillomavirus. At least 80% of women are exposed to HPV during their lifetime. Most HPV infections, including those that are precancerous, typically resolve within 12 months before the virus does any harm. However, HPV infections that persist beyond 12 months increase the likelihood of cancerous lesions, although not all persistent infections progress into cancer. Most cases of cervical cancer are attributable to HPV infection, with HPV 16 responsible for about 50 percent of cases and HPV 18 for 20 percent of cases. Fifteen HPV types are classified as high risk (HPV 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 73, and 82).
Recommendations for screening can be discussed with your health care provider. We at Garden OB/GYN pledge to develop an individualized screening strategy based on your age, medical history, and other pertinent risk factors. We employ the most up-to-date guidelines to ensure the highest quality of patient-centered care.